In the media: Eclectic St. Louis team of doctors, engineers and machinists answers call for emergency ventilators
BRENTWOOD — In late March, amid growing uncertainty about the coronavirus spreading, doctors at Barnes-Jewish Hospital were concerned about the possibility of running out of ventilators, machines that force enriched air into the lungs so people can breathe.
Grim stories were coming out of Italy and New York about decisions being made when faced with depleted equipment.
Prodded by President Donald Trump, some automotive manufacturers changed their production lines to build thousands of ventilators in the United States. But major deliveries aren’t expected to show up at loading docks for months.
Doctors at Barnes-Jewish Hospital and the Washington University School of Medicine wanted to explore more immediate options to meet the local surge of COVID-19 patients. And they wanted options that didn’t rely on the overburdened supply chain.
On March 23, a formal push was made for emergency ventilators designed and built by experts in the St. Louis region who had ready access to parts. An eclectic team of engineers, scientists, doctors and machinists answered the call to action and delivered their first prototype for clinical simulation on Wednesday.
Finishing touches on three more were underway Friday, with the promise that another 100 could be made soon, if needed.
The small team is working together for the first time. Powered by a cumulative pile of advanced degrees and willingness to help, the group has a lot of street cred, perhaps best illustrated by Dennis Mell’s thumb, which was shortened a long time ago by a milling machine.
“I was happy that somebody tracked me down,” said Mell, in charge of automating the new ventilators. “My first thought was there is a lot of complexity, so I hope we have a good team. And hopefully it’s inexpensive enough so we can help more people. I’ve always told people that it doesn’t do any good to design an artificial heart if it costs $100 million or some number that is unachievable.”
Mell grew up working on dairy farms in the Farmington area before studying electrical engineering at what is now Missouri University of Science and Technology in Rolla. He went on to build cash register machines and their electronic components in Ithaca, New York, before returning to Missouri, where he and his wife, Ellen, started a machine shop in their garage in 1997. That shop grew into Custom Technologies, an engineering and manufacturing business here in a nondescript Brentwood industrial park.

The small firm typically makes an assortment of products for other businesses, ranging from food packaging to medical devices to playground equipment, perhaps the most unusual being a blue plastic raccoon face that peeps out of a tree.
Ellen is the chief executive of the family business. Dennis also spends time as a professor of practice at the McKelvey School of Engineering at Washington University.

Both in their 50s, they see themselves as part of the old guard of manufacturing.
“As we have globalized so much, the concept of product design to full manufacturing, it’s not close to home anymore,” said Ellen.
That they design and build under the same roof came in handy with the first emergency ventilator prototype, specifically being able to adapt the electronic controls to the ever changing mechanism.
“It uses less energy than a coffeemaker,” said Dennis.
‘Good, cheap, effective’
Ventilators are like vehicles. There are really nice ones that cost about $50,000 and have lots of features, such as those in intensive care units that are good at keeping patients comfortable. Then there are emergency transport ventilators, the slimmed down versions used by first responders.
The team’s first prototype was built with less than $2,000 in parts. It’s two feet tall and shaped like the rounded head of an alligator. At the base of what would be the brain, there’s a piece of PVC pipe that holds and protects the main component of the machine — one self-inflating resuscitation bag.
Resuscitation bags, which are in plentiful supply in St. Louis, are made of clear plastic and shaped like a small football. In a pinch, paramedics, respiratory therapists and anesthesiologists hand pump the bags to help keep people breathing.
The team made a mechanism to squeeze the resuscitation bag like a hand.
A coffee-mug-shaped motor, supplied by a New York state company, hooks up to linkage that pushes a plunger straight down against the resuscitation bag, which pushes air through a plastic tube that’s supposed to feed into a patient’s windpipe. As the plunger retracts, the bag fills up for another breath.
There are three basic settings: volume, speed and the ratio of inhale to exhale.
“We are not going to get to perfect,” said Jerry Halley, 62, who is overseeing the project. “We want to make sure we get to good enough, cheap enough and effective enough. When Ford and GM really ramp up, they will blow by us. We are trying to fill that middle gap. We can be nimble.”
Halley’s regular job is chief engineer at Tech Manufacturing, a Wright City business that makes structural parts for fighter jets. Custom Technologies in Brentwood was handling the automation and software. The Instrument Machine Shop at the Washington University School of Medicine was doing most of the hardware and assembly.
“We could build 10 next week easily,” Halley said. “It just depends on the feedback from clinicians.”

Philip Bayly, chair of mechanical engineering and materials science at Washington University, who has a hand in the ventilator project, said there are similar efforts going on around the country. He said the prototype built in St. Louis is based on a design from the University of Minnesota, which is similar to another at MIT. The University of Illinois also has proposed a design.
“We are definitely not trying to reinvent the wheel,” said Bayly, 55. “We are making a slightly different version because of the people and the materials that we have available to us.”
‘Five layers of plans’
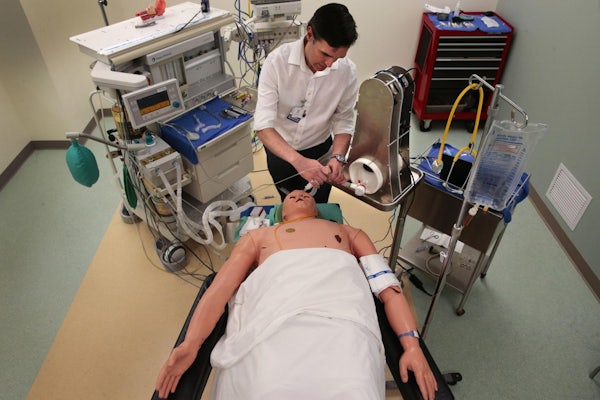
On Wednesday afternoon, Dr. Broc Burke, a former aeronautical engineer who now teaches and practices cardiothoracic anesthesiology at Washington University, picked up the first prototype at Custom Technologies to begin clinical simulation.
Dennis Mell introduced his wife, Ellen, as a physicist who earned advanced degrees in law and business, which come in handy for patents and manufacturing.
“So you, too, lack sanity,” Burke, 44, said about her collection of degrees.
“I find myself telling people, ‘Yeah, yeah, I am a lawyer, but I am nice,’” she said. “I don’t sue people.”
They quickly got down to the basics of how the ventilator works.
Burke saw a couple shortcomings. The possibility to overpressure the lungs and the inability to detect when patients try to take a breath on their own, which is necessary to wean them off ventilators.
They agreed that pop off pressure valves and a separate loop in the controller could address those issues.
“It’s all doable,” said Dennis.
Burke was in good spirits. Based on recent projections for the area, the COVID-19 surge is supposed to peak the end of April. He said BJC is expected to have enough ventilators that are already approved by the FDA.
But he liked the idea of having more options that could be quickly reproduced. He planned to thoroughly test the emergency ventilator version just in case the projections are wrong.
“As an anesthesiologist, we always like to have about five layers of plans,” Burke said.
They packed up the prototype and put it in the back of his SUV. It fit into an open cardboard box that had this printed across the bottom:
Made in the U.S.A., St. Louis, Mo.








